Ultimate Guide to BBT Tracking with PCOS

BBT (basal body temperature) tracking can help you understand your cycle, especially if you have PCOS and experience irregular periods or anovulatory cycles. By identifying post-ovulation temperature shifts caused by progesterone, you can confirm ovulation and gain insights into your hormonal health. Here's what you need to know:
- Why BBT Matters: PCOS often causes irregular cycles and unreliable ovulation predictor kit results due to high LH levels. BBT tracking confirms ovulation by detecting a temperature rise of 0.4°F–1.0°F after ovulation.
- How It Works: Take your temperature every morning before moving or getting out of bed. Look for three consecutive days of higher readings compared to the previous six days.
- Tools: Use a basal thermometer (measures to two decimal places) or wearable sensors like Tempdrop for more consistent results if you have irregular sleep.
- Challenges with PCOS: You may encounter flat charts (anovulation), delayed ovulation, or erratic patterns. Combining BBT tracking with cervical mucus observation or progesterone tests can provide clearer insights.
- What to Watch For: A biphasic pattern (low pre-ovulation temps and higher post-ovulation temps) confirms ovulation. Irregular patterns, short luteal phases, or consistently low temperatures may indicate hormonal issues.
BBT tracking offers a simple, low-cost way to monitor your cycle, manage PCOS, and support fertility goals. Stay consistent, track for at least three months, and consult a healthcare provider if patterns seem unusual.
BBT Tracking Basics
What is Basal Body Temperature?
Basal body temperature (BBT) is your lowest resting temperature, taken right after waking up. It reflects hormonal changes in your body, particularly the rise in progesterone after ovulation [4][5][6][13]. This makes it a reliable way to track hormonal patterns.
For women with PCOS, BBT tracking can confirm ovulation. PCOS affects around 10% of women during their reproductive years, and up to 70% of cases go undiagnosed. By tracking your BBT, you can better understand your hormonal patterns without relying solely on period-tracking apps [12].
BBT can also reveal clues about your metabolism. For example, consistently low pre-ovulation temperatures (below 96°F) could point to thyroid issues - something worth discussing with your doctor [13]. Understanding these patterns helps you get a clearer picture of your cycle.
How BBT Shows Ovulation
After ovulation, the hormone progesterone causes your BBT to rise by about 0.4°F to 1.0°F. For women managing PCOS, this temperature shift is an important signal [5]. Typically, pre-ovulation temperatures range between 96°F–98°F, while post-ovulation readings fall between 97°F–99°F. To confirm ovulation, look for three consecutive days of higher temperatures compared to the previous six days [5].
This method is especially helpful for women with PCOS since ovulation predictor kits (OPKs) can sometimes give false positives due to naturally high LH levels. BBT tracking, which reflects the progesterone increase after ovulation, provides a more accurate way to confirm ovulation [10].
"In PCOS, LH can already be high at baseline, leading to false positives [on OPKs]... This combination of irregular cycles, altered hormone levels, and inconsistent signals makes tracking with PCOS uniquely challenging - but not impossible." - Alex Allan, Nutritionist, PCOS Clinics [10]
If your BBT chart remains flat without any temperature shift, it could indicate an anovulatory cycle, which is common in PCOS. Tracking over time can help you identify patterns and gain better insights into your cycle [14][15].
Common BBT Tracking Myths
Despite being a useful tool, several misconceptions about BBT tracking still exist.
Myth: BBT predicts ovulation in real-time.
BBT tracking doesn’t predict ovulation - it confirms that ovulation has already occurred by showing the progesterone-related temperature rise [1].
Myth: BBT tracking doesn’t work for PCOS.
Even with irregular cycles, long-term tracking can uncover consistent hormonal patterns and confirm ovulation [1][6].
Myth: Missing a day ruins your chart.
Skipping a day or getting an unusual reading due to stress or poor sleep won’t ruin your data. Focus on overall trends rather than individual readings [9].
Myth: Any thermometer will do.
Standard thermometers often measure to one decimal place, but BBT shifts are subtle - sometimes as small as 0.4°F. A basal thermometer, which measures to two decimal places, is essential for accurate tracking [5].
Myth: BBT can act as a pregnancy test.
While 18 days of elevated temperatures may hint at pregnancy, other factors like illness, alcohol, or travel can also raise your temperature. If your readings stay high, take a pregnancy test, but don’t rely on BBT alone [1][9].
Fertility Charting - PCOS | Ovulation Tracking | Pregnancy Chart PCOS
How to Track BBT Accurately
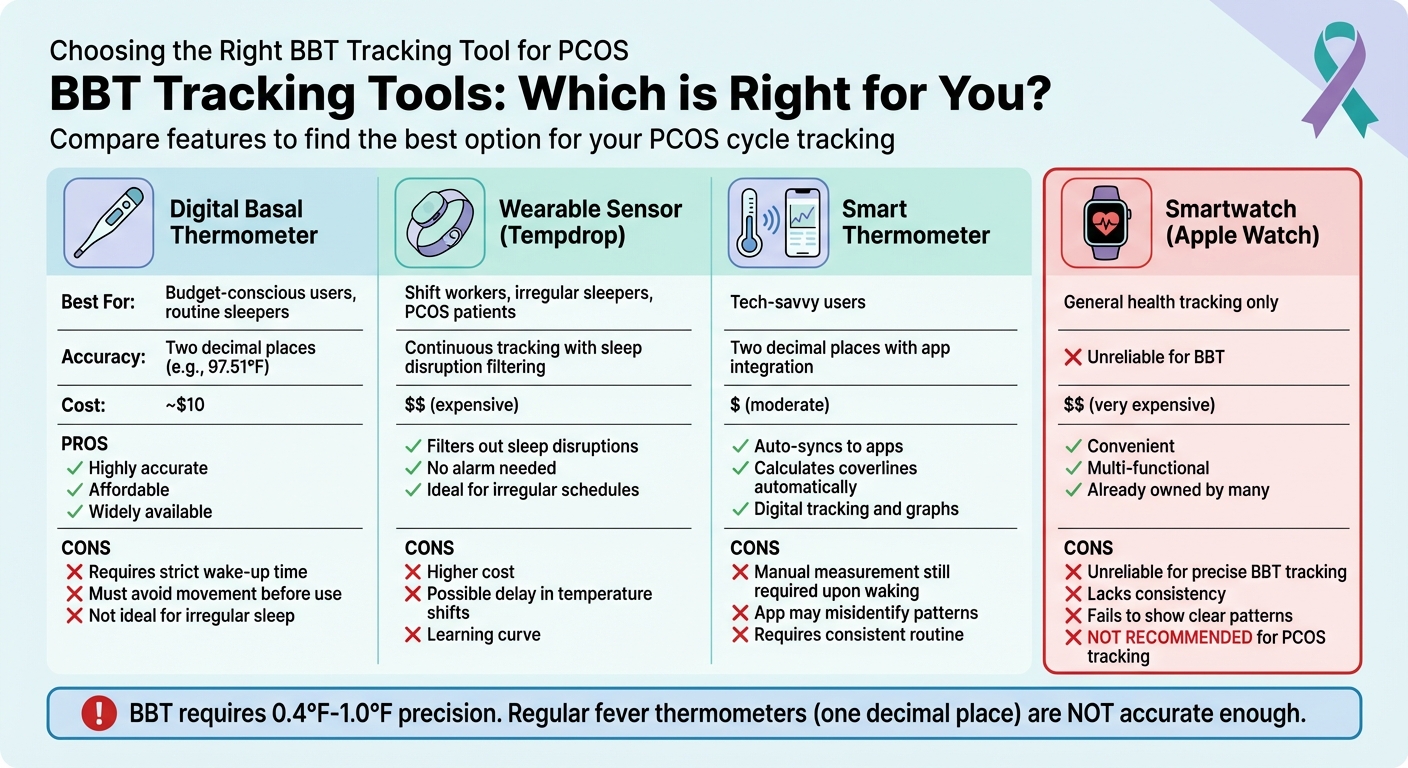
BBT Tracking Tools Comparison for PCOS: Features, Pros and Cons
Choosing Your BBT Tracking Tool
Regular fever thermometers won’t cut it for tracking basal body temperature (BBT). They only measure to one decimal place, while basal thermometers go to two (like 97.51°F), which is crucial for detecting the subtle 0.4°F to 1°F rise after ovulation[1][17].
Digital basal thermometers are often recommended. They’re affordable (around $10 at most drugstores) and reliable, provided you measure at the same time every morning.
For those with irregular sleep patterns, wearable sensors like Tempdrop might be a better option. These devices track your temperature continuously and adjust for sleep disturbances. However, they’re pricier and might show a slight delay in temperature shifts[16][8].
Tech-savvy users might lean toward smart thermometers from brands like Easy@Home or Premom. These sync with apps to graph your data and pinpoint your coverline automatically. But fertility educator Nathalie Daudet warns against relying solely on apps:
"The Premom app misidentified an LH surge by looking at patterns in the LH tests, rather than the individual tests. Had I not been charting mucus and temperature, I would have inaccurately interpreted my chart"[8].
Avoid using smartwatches like the Apple Watch for BBT tracking. In a study of a 48-day PCOS cycle, Daudet found that smartwatch data lacked consistency and failed to show clear patterns, while her oral BBT thermometer provided steady, reliable readings[8].
| Device Type | Best For | Pros | Cons |
|---|---|---|---|
| Digital Basal Thermometer | Budget-conscious, routine sleepers | Accurate and affordable | Requires strict wake-up time; avoid movement before use |
| Wearable (Tempdrop) | Shift workers, irregular sleepers, PCOS | Filters out sleep disruptions; no alarm needed | Expensive; possible delay in temp shifts |
| Smartwatch (Apple Watch) | General health tracking | Convenient; multi-functional | Unreliable for precise BBT tracking |
| Smart Thermometer | Tech-savvy users | Auto-syncs to apps; calculates coverlines | Manual measurement required upon waking |
Daily BBT Tracking Instructions
Start tracking on the first day of your period (the first day of bleeding) to capture your complete cycle[18]. Take your temperature every morning at the same time, sticking to a 30-minute window for accuracy[17][9].
Measure your temperature immediately upon waking - don’t sit up, talk, drink water, or move around, as even minor activity can alter your reading[17][9]. For the best results, ensure you’ve had at least three hours of uninterrupted sleep before measuring[17][7].
Choose one method - oral, vaginal, or rectal - and stick with it throughout your cycle[9]. Record your temperature right away, either manually on a chart or through an app if your thermometer syncs via Bluetooth. Be sure to note any factors that could affect your readings, like illness, alcohol, stress, or disrupted sleep[18][17].
To confirm ovulation, use the "6 and 3" rule: look for three consecutive days of higher temperatures compared to the previous six days[17]. Once you’ve established a routine, focus on minimizing external disruptions for the most reliable data.
Getting Reliable BBT Data
Accurate BBT tracking isn’t just about the thermometer - external factors matter, too. Irregular sleep or frequent wake-ups can cause random temperature fluctuations[9][19]. If consistent sleep is a challenge, a wearable device that filters out disturbances might help.
Room temperature also plays a role. Extreme heat or cold forces your body to work harder to regulate its core temperature, which can skew your readings[9]. Keep your sleeping environment stable and comfortable.
Lifestyle habits impact BBT as well. Limit alcohol and caffeine, especially in the evening, and manage stress to avoid disrupting your readings[9][1].
For those with PCOS, combining BBT tracking with other fertility cues like cervical mucus or saliva ferning offers a clearer picture. PCOS often causes multiple "false start" LH surges, so pairing methods helps differentiate normal hormonal shifts from true ovulation[1][8].
If your pre-ovulation temperatures are consistently low (below 96°F), it might signal a thyroid issue - something worth discussing with your doctor[9].
Managing PCOS-Related BBT Tracking Challenges
PCOS Symptoms That Affect BBT Readings
Tracking basal body temperature (BBT) with PCOS can be tricky, but understanding the specific hurdles can help you navigate them.
One of the biggest issues is anovulation, where no egg is released. Without ovulation, there’s no progesterone surge to cause the typical 0.4°F to 1°F temperature rise, leaving your chart flat[20][21].
Delayed ovulation is another common challenge. While many assume a 28-day cycle, women with PCOS often experience cycles that stretch to 40, 77, or even more days[23][8]. Tracking during these extended cycles requires patience and persistence.
PCOS can also lead to multiple ovulation attempts. Hormonal imbalances may trigger several patches of fertile cervical mucus or LH surges that don’t result in ovulation[20][8]. This can be confusing, as you might see signs of ovulation but no temperature shift - only for it to happen weeks later.
Insulin resistance and inflammation add another layer of difficulty, often causing erratic temperature patterns with zigzags that make it hard to pinpoint a coverline[21][22]. These factors contribute significantly to anovulatory infertility in women with PCOS[22].
Finally, sleep disturbances can throw off readings. Women with PCOS are more likely to experience insomnia or sleep apnea, and less than three to four hours of continuous rest can lead to inconsistent BBT patterns[21][22].
Recognizing these challenges is the first step toward finding practical solutions.
Solutions for Common BBT Disruptions
To tackle PCOS-related BBT challenges, combining methods is key. A symptothermal approach - tracking both BBT and cervical mucus - can be especially effective. While mucus helps predict ovulation, BBT confirms when it has occurred[23][11].
For unclear charts or sluggish temperature shifts, PdG testing (progesterone metabolite urine strips) can confirm ovulation directly, even when your BBT data is noisy or inconclusive[20][21].
If sleep issues are affecting your readings, consider using a wearable sensor like Tempdrop. These devices filter out disruptions from inconsistent sleep, making them a good alternative to traditional oral thermometers, which work best when your sleep schedule is steady[21][23].
To keep your data clean, mark outliers in your app for days when factors like alcohol, illness, or high stress might have skewed your readings. This helps you focus on overall trends rather than getting sidetracked by isolated spikes[21].
| PCOS-Related Disruption | Impact on BBT Tracking | Recommended Solution |
|---|---|---|
| Anovulation | Flat chart with no sustained temperature rise | Use PdG strips to confirm lack of progesterone; consult a provider |
| Insulin Resistance | Erratic temperature readings | Focus on trends, not single days; adjust diet and lifestyle |
| Sleep Apnea/Insomnia | Erratic or inconsistent readings | Use a wearable BBT sensor (e.g., Tempdrop) to account for waking |
| High Baseline LH | False "peak" readings on monitors/tests | Cross-check with mucus observations to verify surges |
| Long Follicular Phase | Delayed temperature shift (e.g., Day 30+) | Keep tracking beyond the expected "fertile window" |
Even small changes, like a 5% reduction in body weight, have been shown to improve PCOS symptoms and cycle regularity[22]. Addressing insulin resistance through diet and lifestyle not only boosts overall health but can also make your BBT charts easier to interpret.
Reading Your BBT Charts
Understanding how to interpret your basal body temperature (BBT) charts is the next step after mastering accurate tracking. This knowledge can help you uncover patterns and gain insights into your hormonal health.
Finding the Coverline and Temperature Shift
Once you’ve gathered several days of temperature readings, the goal is to identify patterns that confirm ovulation. The coverline is a horizontal line placed slightly above the highest temperature recorded during your follicular phase (the first part of your cycle). When you notice three consecutive temperature readings above this line, it signals a temperature shift, which is a reliable sign that ovulation has occurred[26].
"The day before this temperature rise corresponds to the day of ovulation." - Dr. Alexandra MacKillop, Functional Medicine Physician[26]
A healthy BBT chart typically shows a biphasic pattern, meaning two distinct temperature levels: lower temperatures before ovulation and higher ones after. In cases of PCOS, you might see a monophasic chart, where temperatures remain flat without a sustained rise, indicating an anovulatory cycle[1][26].
Keep an eye out for the thermal nadir, the lowest temperature point just before your readings begin to rise. This dip often occurs about one day before ovulation[4][2]. To catch these subtle changes, use a digital basal thermometer that measures to two decimal places (e.g., 98.45°F). Be sure to note any anomalies separately so they don’t confuse your overall pattern[24][26].
For individuals with PCOS, where irregular cycles are more common, these detailed interpretations can help distinguish normal variations from potential health concerns.
Recognizing Patterns and Warning Signs
Your BBT chart can reveal a lot about your hormonal health. For example, irregular patterns with large temperature swings may indicate hormonal instability or external factors like inconsistent sleep[9][1]. A short luteal phase, where elevated temperatures last fewer than 10 days before menstruation, could point to low progesterone or a luteal phase defect[3]. Some charts may show a slow temperature rise, where the increase happens gradually over several days instead of spiking, making it harder to pinpoint the exact day of ovulation[27].
Consistently irregular patterns or abnormal baseline temperatures could suggest conditions like thyroid dysfunction or low progesterone[9][3]. A triphasic pattern, where there’s a second temperature rise 7 to 10 days after ovulation, might indicate implantation or early pregnancy[26]. Additionally, if your BBT stays elevated for 18 days or more after the shift, it’s a strong sign of pregnancy[9][1].
"If BBT doesn't increase or the pattern is erratic, it might indicate hormonal irregularities, like thyroid dysfunction or anovulation." - Inovi Fertility[9]
For reliable insights, track your cycles for at least three months. This helps you establish your personal baseline and makes it easier to spot deviations. Keep in mind, though, that BBT tracking is only about 22% accurate in pinpointing the exact day of ovulation[4][27].
These patterns give you a window into your hormonal health and can guide you toward informed decisions.
Using BBT Data for Health Decisions
Your BBT charts are more than just a way to track ovulation - they’re a valuable resource for discussing your health with your provider and tailoring your wellness approach.
Sharing your charts with your healthcare provider can help identify issues like anovulation, thyroid imbalances, or progesterone deficiencies[9][25]. For example, a luteal phase consistently shorter than 10 days is a clear sign to investigate further and potentially adjust treatment[3]. Flat or erratic charts might prompt additional testing or medication adjustments.
"Interpret your BBT chart as part of a broader picture, and use it in conjunction with other fertility tracking methods for more accurate predictions such as cervical mucus monitoring and ovulation test kits." - Raquel Monroy, Fertility Nutritionist[3]
For those with PCOS, high baseline LH levels can lead to false positives on ovulation predictor kits. Your BBT data can confirm whether an LH surge actually led to ovulation or was a false alarm[8]. Additionally, your charts can reflect how lifestyle changes - like tweaks to your diet, exercise, or supplements - affect your cycle. Even a 5% reduction in body weight has been shown to improve PCOS symptoms and cycle regularity[22], with clearer patterns and more consistent temperature shifts often appearing as a result.
Conclusion
Key Points for BBT Tracking Success
BBT tracking is an effective tool for managing PCOS, especially when you understand its capabilities and limitations. It helps confirm ovulation by identifying the progesterone-driven temperature rise, which is particularly useful when high baseline LH levels lead to false positives on ovulation predictor kits [1][8][17].
To get accurate results, take your temperature consistently each morning as soon as you wake up. Keep a digital basal thermometer (one that measures to two decimal places, like 98.45°F) by your bed for easy access [9][26]. Focus on identifying overall trends across several cycles rather than overanalyzing single readings [1][26].
"BBT tracking depends on consistent, daily data, so in order to see the big picture, look for those 6 lows followed by 3 highs!" - Dr. Patti Haebe, NMD, Senior Medical Advisor, Premom [17]
A healthy ovulatory cycle typically shows a biphasic pattern, with a clear and sustained temperature shift confirming ovulation. On the other hand, a flat chart may signal an anovulatory cycle, which is common with PCOS. Monitor your BBT for at least three months, and note any factors like illness, stress, or disrupted sleep that could affect your readings [1][8][26].
These practices lay the foundation for consistent and accurate cycle tracking.
Getting Started with BBT Tracking
Starting your BBT tracking journey is straightforward and affordable. All you need is a reliable digital basal thermometer and a consistent morning routine to record your temperature immediately upon waking [5][17].
For a more complete picture, combine BBT tracking with cervical mucus monitoring or LH testing. This approach can help confirm whether an LH surge has led to ovulation [6][8][9]. Be patient - identifying your unique patterns often takes three or more cycles, especially if your PCOS causes irregular cycles [1][26].
"By charting basal body temperature, we can learn the exact day on which we ovulate in a given cycle, predict the day of ovulation in a future cycle, and identify our fertile days." - Dr. Alexandra MacKillop, Functional Medicine Physician [26]
Your BBT data offers valuable hormonal insights that can guide conversations with your doctor and support your PCOS management. Start tracking today, stay consistent, and trust that your patterns will reveal themselves over time.
FAQs
How do I confirm ovulation if my temperatures are erratic with PCOS?
Confirming ovulation when dealing with erratic temperatures can feel challenging, but staying consistent makes a big difference. Use a basal thermometer every day at the same time, right after waking up, to get the most accurate readings. It’s also important to maintain steady sleep patterns and healthy lifestyle habits to minimize temperature swings.
To improve accuracy, pair basal body temperature (BBT) tracking with other methods, such as observing changes in cervical mucus or using ovulation predictor kits (OPKs). Tracking over several cycles can reveal patterns, even with the hormonal shifts often experienced with PCOS.
What should I do if my BBT chart stays flat for weeks?
A flat Basal Body Temperature (BBT) chart over several weeks might indicate you're not ovulating or that there are issues with how you're tracking. To get accurate readings, make sure you're measuring at the same time every morning, immediately after waking, using a dependable basal thermometer. Keep in mind that factors like stress, poor sleep, or changes in your surroundings can also affect your results. If your chart stays flat even with consistent tracking, it may be worth consulting a healthcare provider to check on your hormonal health.
When should I talk to my doctor about my BBT patterns?
Consult your doctor if your BBT tracking reveals irregular cycles, consistent absence of ovulation signs, or patterns that might point to hormonal imbalances. These could be signs of underlying health issues, such as PCOS, that may require medical evaluation.
