PCOS and Liver Health: Connection Explained
If you have PCOS, your liver plays a bigger role in managing your condition than you might think. Women with PCOS are up to 4 times more likely to develop fatty liver disease, even if they're not overweight. This happens because PCOS-related issues like insulin resistance and high androgen levels promote fat buildup in the liver, which worsens hormone imbalances and PCOS symptoms like acne, irregular periods, and excess hair growth.
Here's why this matters: Your liver helps regulate hormones, blood sugar, and toxins. When it's not functioning well, it lowers SHBG (a protein that controls testosterone), making PCOS symptoms harder to manage. The good news? Lifestyle changes like exercise, a Mediterranean diet, and targeted supplements (like omega-3s and NAC) can help improve liver health and reduce PCOS-related challenges.
Key Takeaways:
- PCOS increases the risk of fatty liver disease (up to 70% of women with PCOS may be affected).
- Liver dysfunction can worsen PCOS symptoms by disrupting hormone balance.
- Early signs of liver issues include fatigue, abdominal discomfort, and elevated liver enzymes.
- A Mediterranean diet, regular exercise, and supplements like omega-3s can support liver health and improve symptoms.
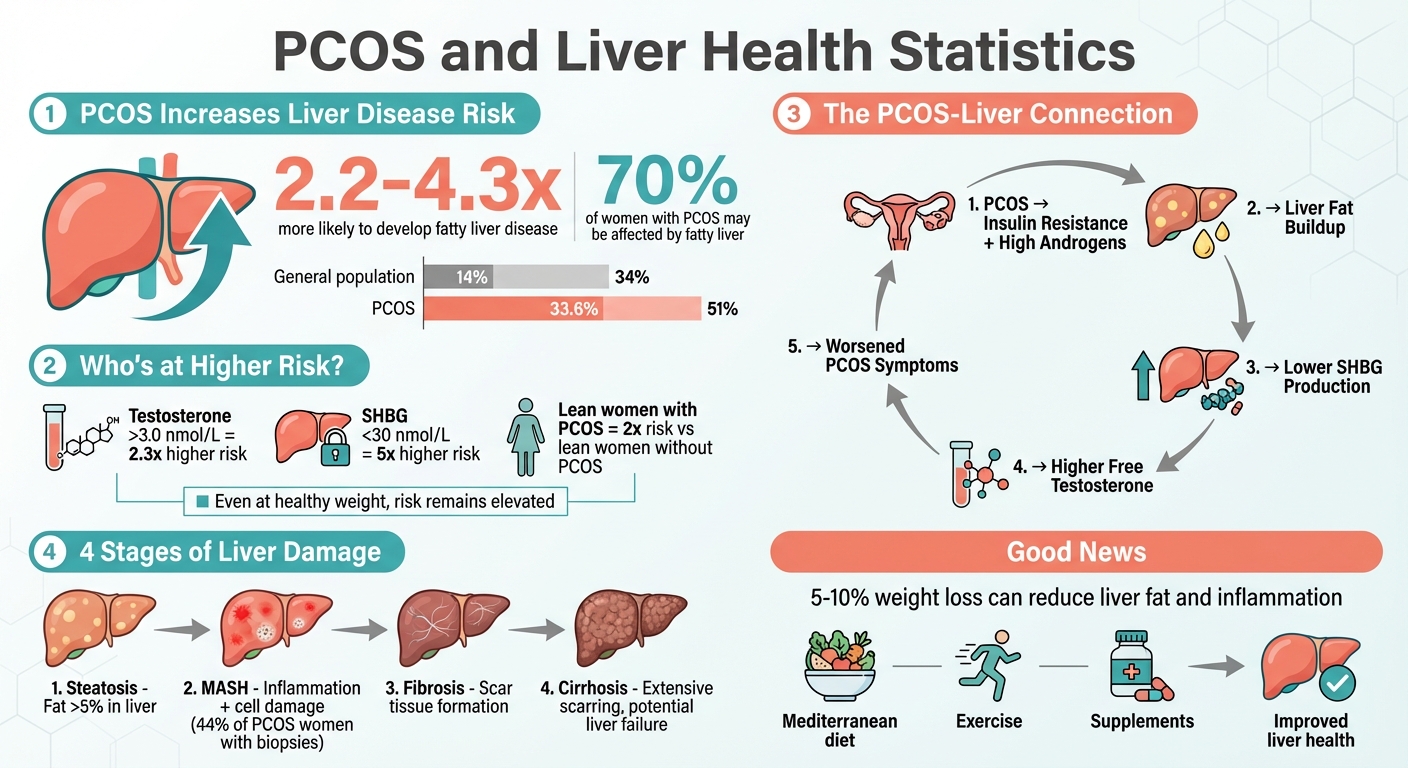
PCOS and Liver Health: Risk Statistics and Key Facts
The Gut–PCOS Connection: Inflammation, Insulin Resistance, and Solutions | Felice Gersh, MD
How PCOS Affects the Liver
Research indicates that women with PCOS have a higher likelihood of developing liver-related health issues. Recognizing how PCOS impacts the liver is key to taking steps to protect it.
PCOS and Fatty Liver Risk
Women with PCOS are 2.2 to 4.3 times more likely to develop fatty liver disease compared to those without the condition, even when weight differences are accounted for [4][9]. One large-scale study revealed that women with PCOS had 4.30 times higher odds of having fatty liver disease than the control group. While fatty liver affects 14%–34% of the general population, its prevalence in women with PCOS ranges from 33.6% to 51%, with some studies showing rates as low as 4.2% in healthy controls [9][12].
This heightened risk isn’t limited to women with higher body weight. Even lean women with PCOS face nearly double the risk of developing fatty liver compared to lean women without the condition [2]. Hormonal imbalances also play a significant role. For instance, women with testosterone levels above 3.0 nmol/L are 2.30 times more likely to develop fatty liver, while those with low Sex Hormone-Binding Globulin (SHBG) levels (below 30 nmol/L) have nearly a fivefold increased risk [2][10].
"In addition to increased BMI and dysglycemia, androgen excess contributes to the development of NAFLD in women with PCOS." – Kumarendran et al., PLOS Medicine [10]
These risks are rooted in the metabolic disturbances associated with PCOS, which are explored below.
What Causes Liver Problems in PCOS
The increased risk of fatty liver disease in PCOS stems from three key metabolic factors: insulin resistance, elevated androgen levels, and metabolic syndrome. Together, these factors create conditions that encourage liver fat buildup.
Insulin resistance is a major contributor. Insulin-resistant fat cells release free fatty acids, which then accumulate in the liver. High insulin levels further exacerbate this issue by promoting additional fat production in the liver [5][7][8].
High androgen levels add to the problem by increasing abdominal fat and reducing protective hormones like adiponectin. Androgens may also directly damage liver cells, accelerating disease progression [4][5][11][12].
Metabolic syndrome, which includes obesity, high cholesterol, and high blood pressure, is another well-documented risk factor for liver disease. Around 80% of women with both PCOS and fatty liver also show central obesity and insulin resistance [9]. Chronic low-grade inflammation, often linked to these conditions, adds even more strain on the liver [5][8].
"Existing data support that NAFLD is the hepatic manifestation of the metabolic syndrome." – Evangeline Vassilatou, MD, PhD, Attikon University Hospital [5]
These interconnected factors highlight how PCOS-related metabolic issues directly compromise liver health. The relationship creates a challenging cycle: PCOS promotes liver fat accumulation, while fatty liver, in turn, worsens insulin resistance, making PCOS symptoms even harder to manage [3][8].
How Liver Problems Worsen PCOS
When the liver is damaged, it sets off a chain reaction that worsens PCOS symptoms. The connection is twofold: PCOS promotes liver fat buildup, and the resulting liver issues disrupt hormone regulation and aggravate metabolic challenges [3][16]. This vicious cycle highlights how liver damage can amplify the struggles associated with PCOS.
Stages of Liver Damage
Liver damage doesn’t happen overnight - it progresses through four key stages if left unchecked. The first stage, steatosis, occurs when liver fat exceeds 5%, but without significant inflammation [1][7]. If this continues, it can progress to MASH (Metabolic Dysfunction-Associated Steatohepatitis, previously called NASH), where fat accumulation causes inflammation and damage to liver cells [1][7]. Persistent inflammation leads to fibrosis, which is the formation of scar tissue in the liver [7][15]. The final stage, cirrhosis, involves extensive scarring that replaces healthy liver tissue, potentially leading to liver failure or cancer [7][15]. Alarmingly, studies show that 44% of women with PCOS who undergo liver biopsies have MASH, compared to 20.8% of women without PCOS [7]. Recognizing the early signs of liver damage is essential as the condition progresses.
Signs of Liver Dysfunction
Liver dysfunction can be a silent issue, often going unnoticed until it’s advanced. One of the earliest signs is chronic fatigue or persistent exhaustion [1][15]. You might also feel discomfort or pain in the upper right part of your abdomen, along with nausea [1][15]. Blood work can reveal elevated levels of liver enzymes like ALT, AST, and GGT, which are common indicators of liver stress [9][7][1]. Another clue is acanthosis nigricans, dark, velvety patches of skin often found around the neck or armpits, which point to insulin resistance driving liver fat [14][1]. In more advanced cases, symptoms like jaundice (yellowing of the skin or eyes) and swelling in areas such as the abdomen, legs, or feet may appear [1]. Interestingly, liver fat can exist even when enzyme levels are normal, making it tricky to detect without further testing [9][1].
Effects on Hormones and PCOS Symptoms
The liver plays a vital role in producing SHBG (sex hormone-binding globulin), and when it’s not functioning properly, hormonal imbalances worsen. A damaged liver produces less SHBG, leading to higher levels of free testosterone. This can amplify PCOS symptoms, including hirsutism, acne, and irregular ovulation [7][3]. Additionally, a damaged liver releases hepatokines like Fetuin-A and Fetuin-B, which interfere with insulin receptors [3]. This worsens insulin resistance, which in turn drives androgen production, further escalating PCOS symptoms [7][3]. Poor liver function also affects fat metabolism, contributing to abdominal fat and weight gain [7][1]. On top of that, a stressed liver increases the production of pro-inflammatory cytokines such as IL-6 and TNF-α, fueling the chronic inflammation often seen in PCOS [13][7][16].
"Whilst it is recognized that PCOS may contribute to hepatic dysfunction, there is also evidence that the liver may contribute to the features of PCOS... with a potential bidirectional relationship." – Biomolecules [3]
How to Support Liver Health with PCOS
Liver damage associated with PCOS can often be reversed with targeted efforts. For instance, losing just 3% to 5% of body weight can reduce liver fat, while a 7% to 10% loss can help decrease inflammation and scarring [1][15]. By combining lifestyle changes, dietary tweaks, and specific supplements, it's possible to create a healthier environment for both liver function and hormone balance. Here’s how you can approach it.
Lifestyle Changes for Liver Health
Making lifestyle changes that reduce liver fat can also improve insulin resistance and hormonal imbalances tied to PCOS. Physical activity is a key player here. Regular exercise - 150–300 minutes of moderate activity or 75–150 minutes of high-intensity workouts weekly - can significantly reduce liver fat, even without major weight loss [1]. Adding resistance training twice a week can further enhance how your body processes glucose and fat [18][20].
Sleep and stress management are equally important. Aim for 7–9 hours of sleep each night and practice stress-reducing techniques like mindfulness to help regulate hormones [1][19]. Staying hydrated (8–10 glasses of water daily) and eating sulfur-rich foods like garlic and onions, along with bitter greens, can also support liver detoxification [17][19].
Diet Changes for Liver Support
A Mediterranean-style diet is particularly effective for improving liver health and reducing inflammation. Focus on nutrient-dense foods such as fatty fish, avocados, olive oil, nuts, leafy greens, and whole grains [17][18]. Incorporate low-glycemic foods like quinoa, barley, and lentils to stabilize insulin levels and reduce fat storage [20].
Avoid added sugars, especially high-fructose corn syrup, as well as refined carbs and processed meats, as these can contribute to liver fat accumulation [1][17][20]. Foods rich in omega-3s, such as walnuts and flaxseeds, can protect liver cells from oxidative stress, while soluble fiber from oats and apples helps bind dietary fats. Interestingly, an 8-hour eating window (a form of intermittent fasting) over six weeks has been shown to reduce ALT liver enzyme levels in women with anovulatory PCOS [7]. These dietary strategies work hand in hand with the supplements outlined next.
Supplements for Liver and PCOS
Certain supplements can support liver function and help manage PCOS symptoms. For example, omega-3 fatty acids (from fish oil) at a dose of 4 grams daily for eight weeks have been shown to reduce liver fat and triglycerides significantly [21]. Berberine is another option, as it helps prevent fat buildup and promotes fatty acid oxidation, lowering liver enzymes and triglycerides [21].
N-acetylcysteine (NAC), at 1,200 mg daily over three months, can reduce oxidative stress and improve liver function tests [21]. Milk thistle (silymarin) offers anti-inflammatory benefits, with studies showing that 140 mg daily for two months can lower liver enzymes more effectively than metformin in individuals with NAFLD [21]. Vitamin E (800–1,000 IU daily) has been used to reduce liver inflammation and fat, though high doses should be monitored by a healthcare provider [21]. Additionally, vitamin D supplementation (3,200 IU daily for three months) has been linked to lower ALT levels [7].
"Non-alcoholic fatty liver disease (NAFLD) in women with PCOS is common and serious, but can easily be reversed with nutrition and lifestyle changes." – Angela Grassi, MS, RDN, LDN, PCOS Nutrition Center [21].
Comparing Treatment Options
The Mediterranean diet stands out for its ability to reduce liver fat, improve insulin sensitivity, and lower inflammation [1][18]. Low-glycemic foods also play a role by stabilizing insulin levels, which can aid ovulation and reduce androgen levels [20]. Among supplements, omega-3s (at 4 grams daily) not only help reduce liver fat and triglycerides but also lower inflammation and testosterone levels [18]. Berberine supports healthy glucose and lipid metabolism, while milk thistle has been shown to improve insulin resistance and lower liver enzymes more effectively than metformin in some studies [18]. NAC, on the other hand, helps combat oxidative stress and supports liver function by boosting glutathione production [18].
Combining dietary changes, consistent exercise, and carefully selected supplements offers a well-rounded approach to improving liver health and managing PCOS. Together, these strategies can help create a healthier balance for both metabolic and hormonal systems.
Conclusion
The link between PCOS and liver health is more intertwined than many might think. Your liver plays a central role in regulating hormones like testosterone by producing SHBG and managing blood sugar levels [16][22]. When insulin resistance sets in, it can lead to liver fat buildup, worsening hormone imbalances and intensifying PCOS symptoms such as acne and irregular periods [3][4].
The good news? Liver damage associated with PCOS can often be turned around with manageable lifestyle changes. Even a modest weight loss of 5% to 10% can reduce liver fat and inflammation [1][6]. Incorporating a Mediterranean diet, staying active, and using targeted supplements can create a strong foundation to combat liver-related PCOS challenges.
"The liver is the metabolic hub of the body... pathological changes in the liver may contribute to female endocrine disruption, potentially through the liver-to-ovary axis." – Muhammad Sohaib Khan, College of Pharmacy and Integrated Research Institute for Drug Development [16]
Partnering with your healthcare provider is essential to tailor a plan that works for you. Consider requesting annual liver function tests like ALT and AST, especially if you have insulin resistance [17]. Your doctor can also evaluate whether medications such as Metformin or GLP-1 receptor agonists could help and ensure any supplements are used safely. Since as many as 70% of women with PCOS may experience some level of fatty liver - even if they’re at a healthy weight [17][21] - routine screening is crucial for early detection.
Start small. Add more leafy greens to your meals, take a 30-minute walk, or schedule a check-up with your doctor. These simple, consistent actions can gradually improve both your liver health and PCOS symptoms, creating a path toward better overall well-being.
FAQs
Should I get screened for fatty liver if I have PCOS?
If you have PCOS, it’s worth considering a screening for fatty liver. Studies highlight a strong connection between PCOS and nonalcoholic fatty liver disease (NAFLD). Detecting it early can help manage liver-related issues and may also play a role in maintaining better hormone balance.
What tests check liver health and fatty liver?
Liver health, including the presence of fatty liver, is typically evaluated using blood tests. Among these, the alanine aminotransferase (ALT) test stands out, along with other liver function tests. These tests measure enzyme levels and provide insights into how well the liver is functioning.
Can improving my liver lower testosterone symptoms?
Improving liver health can play a role in managing testosterone-related symptoms in PCOS. When the liver functions better, it can reduce fatty liver issues and promote a more balanced metabolism. Since these factors are connected to excess androgen production, supporting liver health may aid in regulating hormones and enhancing overall well-being.
